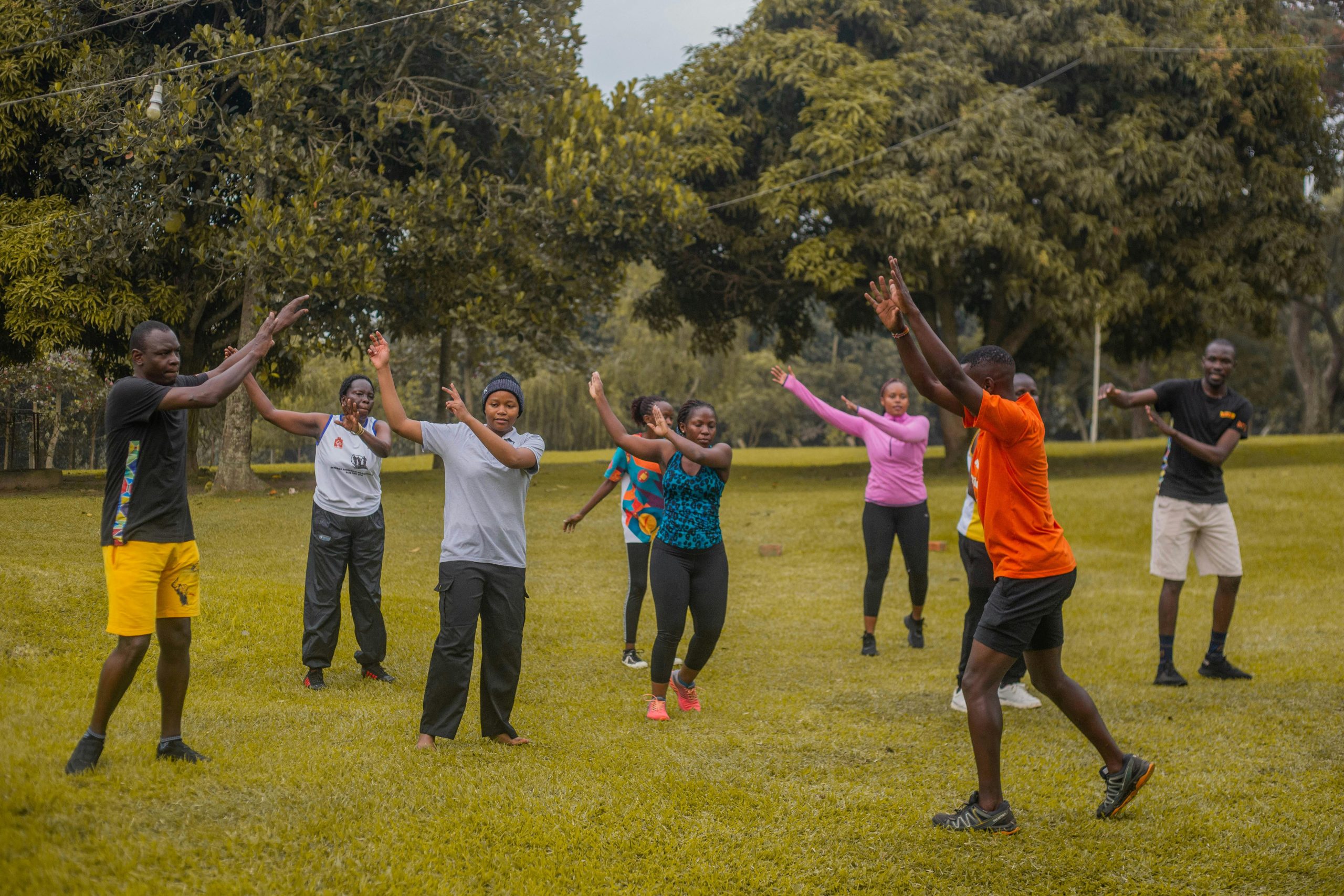Worried about memory slips in yourself or a loved one? With so many supplements, apps, and “miracle” claims online, it’s hard to know what actually helps. The good news is that science has made real progress.
Memory treatment today focuses on two main approaches: addressing underlying causes when possible and using proven strategies to support or improve cognitive function. While there is still no cure for most memory disorders, strong evidence supports certain lifestyle changes, cognitive interventions, and — in specific early cases — disease-modifying medications.
In this post, we’ll review what current research (including major 2025 studies like U.S. POINTER) actually supports for memory issues ranging from normal age-related changes to mild cognitive impairment (MCI) and early dementia.
Understanding Memory Problems Today
Memory difficulties can stem from many causes: normal aging, stress, poor sleep, medications, ADHD/learning disabilities, mild cognitive impairment, or early Alzheimer’s/vascular issues. Accurate diagnosis through neuropsychological testing (as we discussed earlier) is the essential first step before choosing any treatment.
Strongest Evidence: Multimodal Lifestyle Interventions
The most consistent and accessible evidence supports structured lifestyle changes that target multiple risk factors at once.
- U.S. POINTER Trial (2025): This large randomized study of over 2,100 older adults at risk for cognitive decline found that a structured program combining physical exercise, MIND diet (brain-healthy nutrition), cognitive and social engagement, and cardiovascular health monitoring significantly improved global cognition over two years. Benefits were greater with a more structured/supportive approach than self-guided changes.Alz
Similar results from the earlier FINGER trial and other studies confirm that consistent physical activity, healthy eating, mental stimulation, and social connection can improve cognition and help protect against decline.
Key supported components:
- Physical Activity: Aerobic exercise, resistance training, and mind-body practices (yoga/tai chi) improve memory, executive function, and overall cognition. Even moderate activity several times per week shows benefits across all ages.Bjsm.bmj
- Nutrition: MIND or Mediterranean-style diets rich in berries, leafy greens, fatty fish, nuts, and olive oil support brain health and may slow decline.
- Cognitive & Social Engagement: Mental challenges (puzzles, learning new skills) and regular social interaction build cognitive reserve.
- Sleep, Stress Management & Vascular Health: Treating sleep issues, managing stress, and controlling blood pressure, diabetes, and cholesterol are foundational.
These changes are safe, low-cost, and beneficial even without a formal diagnosis.
Cognitive Training and Stimulation
Computerized cognitive training, group cognitive stimulation therapy, and strategy-based training show modest but meaningful benefits, especially for attention, working memory, and global cognition in people with MCI.
- Effects are often stronger when training is combined with physical exercise (motor-cognitive training).
- Reminiscence therapy and structured cognitive stimulation may help global cognition across stages of impairment.
- Gains are typically greatest on trained tasks but can transfer modestly to daily functioning when programs are well-designed.
Results vary by intensity, duration, and individual factors — structured programs with professional guidance tend to work better than casual app use.
Medications and Disease-Modifying Therapies
For symptom management (especially in Alzheimer’s or related dementias):
- Cholinesterase inhibitors (donepezil, rivastigmine, galantamine) and memantine can provide modest, temporary improvements in memory and daily function for some people.
- These do not stop disease progression but may help for 6–12 months or longer in certain individuals.
For early Alzheimer’s disease (mild cognitive impairment due to AD or mild dementia):
- Anti-amyloid monoclonal antibodies like lecanemab (Leqembi) and donanemab (Kisunla) are FDA-approved disease-modifying treatments. They clear amyloid plaques and slow cognitive decline by about 30% in early stages. These require biomarker confirmation (PET scan or blood test) and careful monitoring for side effects (ARIA — brain swelling or bleeding).Mayo Clinic
These represent a major advance but are not suitable for everyone and work best when started early.
Other experimental therapies (brain stimulation, new small molecules, etc.) are in trials but not yet standard treatment.
What Has Limited or Mixed Evidence
- Many over-the-counter supplements (ginkgo, omega-3s alone, vitamins) show weak or inconsistent results for memory improvement.
- Standalone “brain training” apps without structured support often produce limited real-world transfer.
- Unproven “memory boosters” or unvalidated therapies should be approached with caution.
Always discuss supplements or new treatments with a doctor, as some can interact with medications.
Practical Next Steps
- Get a proper evaluation — Neuropsychological testing helps identify the cause and map strengths/weaknesses.
- Start with lifestyle fundamentals — Prioritize exercise, nutrition, sleep, stress reduction, and social engagement (see our earlier posts on these topics).
- Consider structured programs — Multimodal interventions (like those in POINTER) offer the strongest evidence.
- Work with specialists — Neurologists, neuropsychologists, or geriatricians can guide personalized plans, including whether medications are appropriate.
- Create supportive environments — Use memory-friendly home setups and routines to reduce daily frustration.
Final Thoughts
Memory treatment today is more promising than ever. While dramatic cures are not yet available, robust science supports multimodal lifestyle interventions as a powerful first-line approach for many people. For those with early Alzheimer’s pathology, disease-modifying therapies offer new hope to slow progression.
The most effective strategy usually combines several evidence-based elements: regular physical activity, brain-healthy eating, cognitive and social stimulation, good sleep, and medical management when needed. Small, consistent changes — started early — can make a meaningful difference in preserving memory and quality of life.
Talk to your doctor or a specialist about what combination might work best for you or your loved one. You’re not powerless — science-backed tools are available right now.